
News


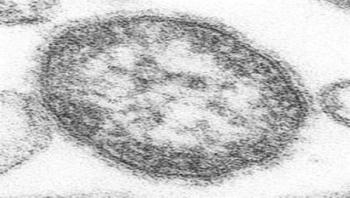
Gary W. Procop, MD, FCAP, a fellow of the College of American Pathologists, explains that measles is characterized by the three Cs: cough, coryza and conjunctivitis. This is followed by a maculopapular rash that usually develops 14 days after the child is exposed, spreading from head to trunk and then to the extremities. When the rash appears, the measles virus can spread.



Slips, trips, falls and sharps are widely recognized as potential occupational risks in the healthcare industry. However, there is another dangerous hazard that often goes unnoticed and underreported-splashes.




Johnson & Johnson (J&J) has donated the published proceedings from conferences on sterilization of medical products to the Association for the Advancement of Medical Instrumentation (AAMI), which will make the material available online as a complimentary service to the sterilization community.


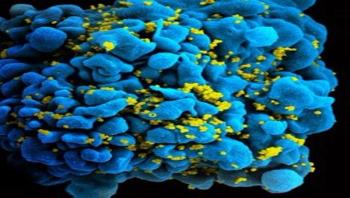
If the human immunodeficiency virus (HIV) is a bit like a hermetically sealed tin can no one has yet been able to break open, the good news is that researchers at the CHUM Research Centre, affiliated with the University of Montreal, have identified a way to use a “can opener” to force the virus to open up and to expose its vulnerable parts, allowing the immune system cells to then kill the infected cells.



In Ebola-affected countries, like Sierra Leone, the lack of running water can make hand hygiene a challenge. Hand hygiene is so important in public health that May 5 every year is marked as Hand Hygiene Day. Dr. Komba Songu-Mbriwa is a doctor on the frontlines of the Ebola fight in Sierra Leone who also knows the challenges of the disease firsthand. He is an Ebola survivor. But today, he says his most important role extends beyond Ebola as a protector of other health workers. His specialty: teaching his colleagues how to protect themselves and other patients from the spread of all infectious diseases when patients are being cared for in health facilities.





Following yet another highly publicized patient exposure to dangerous pathogens via contaminated endoscopes, the healthcare and sterile processing communities are examining their processes, re-evaluating their priorities, and digesting new guidelines issued by several federal agencies.

Contamination. Outbreak. Infection. These are words no healthcare facility wants to hear - especially when they are linked with events that have occurred within their own institutions.

Central Service (CS) professionals who continue to hold out on becoming certified until their state legislators or hospital executives require it are not doing themselves, their healthcare customers and, especially, their patients any favors. Also, as more states board the certification bandwagon and new technicians are required to become certified in order to hold a position in the CS department, more tenured, non-certified professionals – even those who were “grandfathered” in under state law* (meaning that the bill exempts them from having to become certified) – will likely feel the pressure and may lose out to their certified counterparts.

The field of sterile processing is awash with new technologies, ever-tightening accreditation requirements, and an overwhelming flood of cutting-edge surgical instrumentation. But are departmental certification standards and training programs keeping up with these growing trends?


