We must treat this strain with the respect it deserves, but we must not panic. There is no doubt that increased infectivity equates with increases in deaths, but it does not mean the vaccines will not work.

KEVIN KAVANAGH, MD, is the founder of the patient advocacy group Health Watch USAsm, a member of the Infection Control Today's® Editorial Advisory Board, and a frequent contributor to Infection Control Today®.
Health Watch USAsm 2023 Webinar:
Long COVID: Patients, Workers & Society Webinar.
Webinar on Nov. 1, 2023. No charge for viewing or obtaining continuing education credits. CE planned and applied for ANCC Nursing, Physician Cat I ANA along with a number of other allied health professions.
Speakers Include:
Ambassador Deborah Birx, MD, past White House Coronavirus Coordinator. Presentation: "Impact of Long COVID on the United States. "
Pam Belluck, New York Times Reporter -- Presentation: "How Long COVID is affecting people's jobs and their needs at work."
Peter Hotez, MD, PhD, Dean of the National School of Tropical Medicine and Professor of Pediatrics and Molecular Virology & Microbiology at Baylor College of Medicine. will present on "Global Vaccines and Vaccinations: The Science vs The Anti-science."
Conference Objectives:
After attending the sessions about Long COVID, the participants will be able to:
* Describe the manifestations of Long COVID in different age groups.
* Discuss the different presentations of Long COVID.
* Identify the impacts of Long COVID on the healthcare workforce.
For more information go to: https://healthconference.org/
Agenda: https://www.healthconference.org/healthconference.org-files/2023Conference_downloads/_Agenda-3.pdf
Speaker's Bios: https://www.healthconference.org/healthconference.org-files/2023Conference_downloads/_Bios-Speakers-2023-HWUSA-Conference-9.pdf
Download Brochure: https://www.healthconference.org/healthconference.org-files/2023Conference_downloads/20231101-HWUSA_Brochure-5.pdf
Conference Registration - Space is limited:https://docs.google.com/forms/d/e/1FAIpQLSc3sHSOLLNNBwAXcDJlJo5NcuknMexia6H-0SsXJbjmK5YbFQ/viewform
Continuing Education:
Four AMA PRA Category 1 Continuing education credit hours have been approved for Physicians, Nursing Home Administrators and PA/Nurse Practitioners. The Kentucky Board of Nursing has approved the course for 4.8 credit hours. Through the corresponding Kentucky agency/board, Dentistry, Physical Therapy and EMS has been approved for 4 credit hours. Respiratory, Occupational Therapy, Social Work, Dietitian and Community Health Worker approval is pending.
American Nurses Credentialing Center (AANC) approval for 5 hours of continuing education is pending (Connecticut Nurses Association).
For more information, go to: https://healthconference.org/

We must treat this strain with the respect it deserves, but we must not panic. There is no doubt that increased infectivity equates with increases in deaths, but it does not mean the vaccines will not work.

V-Safe and VAERS are 2 monitoring systems for patients who are given a COVID-19 vaccine. Infection preventionists can play a vital role in educating about the strengths and drawbacks of each.
Infection preventionists are an important component of fostering trust in the healthcare system and need to actively articulate to both patients and on social media the need to be vaccinated and to follow public health advice.

Faced with greater than three times the number of cases as the last surge, along with exponential growth with no end in sight, there is little hope healthcare workers can safely treat patients without a drastic change in policy and a more productive and secure supply line.
The worst-case scenario is that if an effective and safe COVID-19 vaccine is found, a large segment of our population will elect to use hydroxychloroquine or another ineffective treatment instead, allowing the virus to continue to thrive, and devastate our nation.

By their nature, challenge trials have to be performed in young healthy individuals. SARS-CoV-2 is most lethal in the elderly and those with co-morbidities. Thus, an effective vaccine may be found for the young, but not in the elderly with an aging immune system.

For infection preventionists and frontline healthcare workers, the Great Barrington Declaration places their lives and livelihood at risk. A field hospital has been activated in Wisconsin and the state is at risk of running out of hospital beds and trained staff.

The real impact of these recommendations are what they mean for aerosolization, outdoor gatherings of any type and food handling practices.
Patients afflicted with COVID-19 have an increased susceptibility to antibiotic resistant infections both from prolonged hospitalizations and the use of immunocompromising agents such as dexamethasone.
It is imperative that infection preventionists engage and combat this messaging on social media and wherever it occurs. To not do so, allows misinformation to fan the pandemic, placing all of our lives at risk.
Infection preventionists need to be able to articulate to those who feel that the young are safe just because their fatality rate is extremely low, that even in this age group there are major concerns regarding long-term consequences of this virus.
This year we have to do more than just rely on the flu vaccine. Avoiding the flu plus COVID-19 catastrophe is contingent on the US widely embracing public health guidance of wearing masks, meticulous hand hygiene and social distancing.

Infection preventionists are of utmost importance to work with school systems and provide the safest strategies and environmental modifications which can suppress the transmission of the SARS-CoV-2 virus.

The resources used to study hydroxychloroquine (HCQ) would have been better spent on more promising treatment modalities, such as studying Camostat mesilate or nafamostat mesylate therapy for COVID-19, a compound which has been shown to block TMPRSS2.

After decades of reluctance to implement a national reporting system, when COVID-19 came along we witnessed almost overnight the formulation of case definitions and comprehensive national reporting from all healthcare facilities.
COVID-19 cases in many states have risen and the false narrative is that this is because of increased testing. But the rise in cases far outstrips the rise in testing.

Infection preventionists (IPs) are stretched to the limit with both reporting and patient responsibilities with an unwillingness of facilities to prioritize infectious disease prevention in their operating budgets.

Viral droplets from a sneeze can even travel 23 to 27 feet.

These pathogens are relentless, they are evolutionarily programed to win, and they are currently doing just that.
Just because we declare the economy open does not mean it will. It is treated as a switch, but it is not.

We are forced to act on best evidence, but in some cases the evidence is less than actionable.

The CDC’s recommendation of using a bandana as a last resort to stop the COVID-19 virus places our healthcare system at the level of a third-world country and underscores the severity of the current pandemic and erosion of our healthcare system’s infrastructure.

At a hospital that recently announced layoffs during the COVID-19 crisis, hospital executives agreed to a 20% pay cut. That sounds impressive but the CEO makes over $1.9 million a year and the corporation has net assets or fund balances of $1.6 billion. Meanwhile, the shortage of N95 face masks for healthcare workers continues.

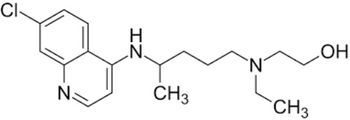
If you are on one of these medications one should perform strict social distancing and protect yourself from contracting COVID-19.

In Washington State, a choir practice of 60 individuals who practiced social distancing resulted in 45 infections, 3 hospitalizations and 2 deaths.
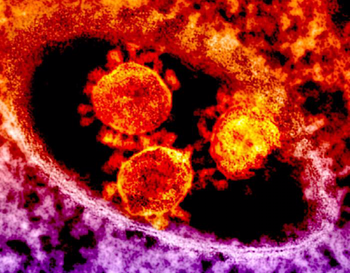
ACE inhibitors up regulate (increase) the ACE2 receptor. This is the receptor the COVID-19 virus uses to attack the lungs.
There are far too few trained staff assigned to infection control. IPs do not even have time to document and report infections let alone evaluate patients and conduct training.

Already, two emergency room doctors in the United States are in critical condition with COVID-19.

A CNN commentator made the alarmist statement that we may get to the point where the national guard is escorting patients to a high school gym for placement on ventilators. This is of course a ridiculously misinformed statement since we do not have enough ventilators.