News


Enhancing quality, promoting patient safety and ensuring value is the healthcare industry's current trifecta, but there are many more imperatives from a regulatory perspective, including shifting from volume-based to value-based reimbursement, enhancing transitions and reducing hospital readmissions, and improving patient satisfaction and engagement. In concert with these efforts comes the prevention of adverse events and infections. In today's environment of transparency and reform, understanding legal liability for healthcare-acquired infections (HAIs) is more critical than ever for infection preventionists as they assist their risk managers and patient safety officers with quality improvement initiatives.

Twenty years ago, the Institute of Medicine (IOM) identified major inconsistencies in the way high quality medical care is delivered to the masses. They called for sweeping action and talked about its vision for the future in a report titled “Crossing the Quality Chasm.” Many of us were young ourselves in our understanding of quality improvement. Two leading approaches – W. Edwards Deming’s model of Total Quality Management and Joseph Juran’s work for continuous quality improvement – were being studied with attempts to adapt them into the healthcare setting.




In a light-filled lab at the Food and Drug Administration (FDA), a collection of small containers are growing the bacteria that cause whooping cough.




St. Jude Children’s Research Hospital scientists have discovered how pieces of bacterial cell wall cross the placenta and enter developing neurons, altering fetal brain anatomy and cognitive functioning after birth. The study appears today in the scientific journal Cell Host & Microbe.
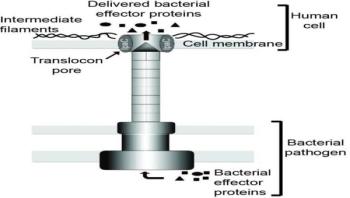
Researchers from the Massachusetts General Hospital (MGH) Division of Infectious Diseases are investigating the mechanism by which several important pathogenic species of bacteria deliver proteins into the cells of the organisms they are infecting. In a paper receiving advance online publication in Nature Microbiology, the team describes determining a key step in how the diarrheal pathogen Shigella injects proteins into target host cells. Their findings may apply to additional bacterial species, including Salmonella and those responsible for typhoid fever, bubonic plague and many hospital-acquired pneumonias.







The second meeting of the Emergency Committee (EC) convened by Margaret Chan, MD, the director-general of the World Health Organization (WHO) under the International Health Regulations (2005) (IHR 2005) regarding clusters of microcephaly cases and other neurological disorders in some areas affected by Zika virus was held by teleconference on March 8, 2016.