HAIs
Latest News
Latest Videos
More News

In this provocative interview, Kevin Outterson, JD, LLM, explains why infection prevention benefits society but costs hospitals, urging fire department–style funding and PASTEUR incentives that reward diagnostics, stewardship, and antibiotic use.
For more than 80 years, the humble chicken egg has quietly powered one of modern medicine’s most vital defenses: vaccines. Even in an age of recombinant DNA, mRNA platforms, and cell-based innovations, more than 80% of the world’s influenza vaccines still begin in an egg. The process is time-tested, affordable, and reliable—but also imperfect. read this to learn more.

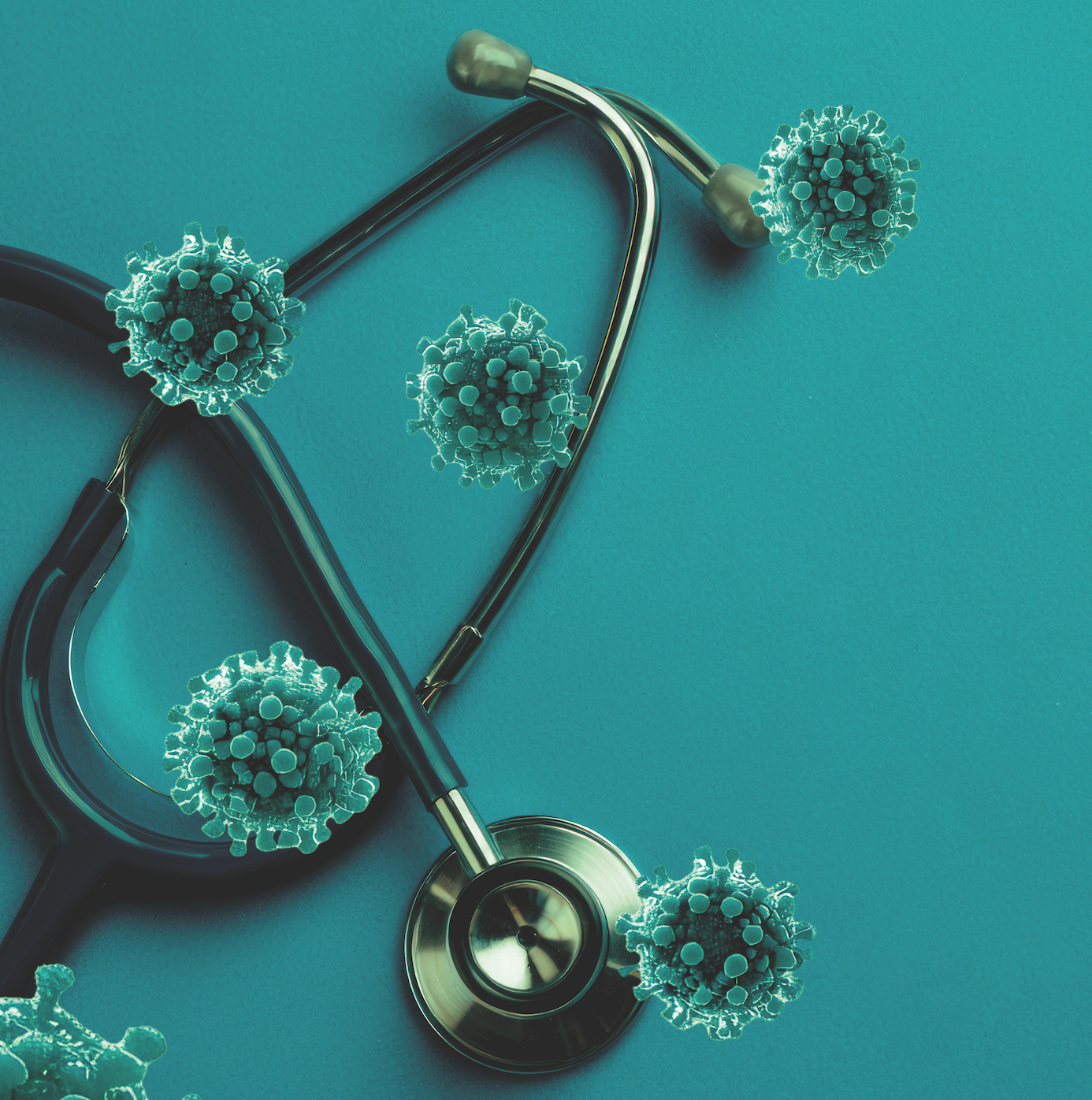
Much is discussed about stethoscopes, the "third arm" of clinicians, but what about the risk of spreading health care-associated infections?

With hospitals across the country accelerating investments in automation, why does human competence remain vital?

Dental and oral surgery clinics are often overlooked in infection prevention programs, yet lapses can have serious consequences. Strengthening surveillance, sterilization, and patient safety practices is critical to reducing surgical site infections.

Elevating IPs into executive leadership isn't symbolic; it's a strategic imperative.

The November/December 2025 issue of Infection Control Today® dives into overlooked risks, breakthrough technologies, and the people driving innovation across IPC, EVS, and sterile processing. From bacteriophage therapy to burnout prevention, automation to UV regulation—it’s a powerful close to the year. Read the issue now: https://www.infectioncontroltoday.com/journals/infection-control-today #InfectionPrevention #Healthcare #InfectionControl #EVS #IPC #PatientSafety #ICT

Oman is earning international attention for transforming hospital environmental hygiene into a national success story. Through the Clean Hospitals initiative, updated cleaning contracts, and workforce training, the Ministry of Health is showing how a unified approach to cleaning, auditing, and accountability can reduce infection risk and raise global standards in health care hygiene.

After nearly a decade of research and regulatory review, the US Environmental Protection Agency (EPA) has determined that Micrillon, a polymer-based antimicrobial additive developed by UMF Corporation, is not a pesticide—clearing the way for new infection prevention applications. In this interview, UMF President George Clarke and Editorial Advisory Board member Heather Stoltzfus, MPH, RN, CIC, discussed how this rechargeable technology could redefine cleaning, sustainability, and surface safety across healthcare and hospitality settings.

The Bug of the Month helps educate readers about clinically significant pathogens, both existing and emerging, in today's health care facilities.

Sherrie is back! In this The Clean Bite, she discusses single-use vs Resusable Dental Supplies. Ultrasonic scaler tips, burs, and endodontic files are often reused despite being marketed as single-use. How many patients are at risk from shortcuts in reprocessing?

"Hospital tray lines operate at high speed to feed hundreds of patients daily. Staff members plate food, cover trays, and load them onto mobile carts that navigate elevators, hallways, and patient rooms. Each of these steps introduces opportunities for contamination."

I’ve known Monica and Tim forever, which is why their sepsis battles aren’t just “patient stories” to me. They’re a reminder that infection hides in ordinary days, and that vigilance, source control, and smart antibiotics save lives.

Infection prevention��’s future will be won with mentorship, soft skills, and honest collaboration—not just guidelines. In a candid roundtable, veteran IPs shared how to steady first-year practitioners: pair them with real mentors, teach time management and tough conversations, and build cultures that value “let me confirm” over guesswork.

This 6-part series will chronicle the journey of 2 infection prevention leaders, Brenna Doran, PhD, MA, ACC, CIC; and Jessica Swain, MBA, MLT, CIC, IHI, as they partnered to research and shed light on the critical issue of infection prevention staffing in the current health care landscape. From the initial spark of an idea to the publication of an impactful article, a research manuscript, and a podcast, this series will offer an insider’s view of their collaborative process and the profound implications of their findings. This third article in the series will focus on...

If you’ve ever been asked to track flu shots and handle a chemical splash in the same breath, you’ve met the IP–OH blur. Infection prevention and occupational health often intersect—but their missions differ. Knowing where each begins ensures safer patients, safer staff, and smoother responses.

When a nationwide blood-culture bottle shortage squeezed hospitals, a Stanford-led team turned to machine learning by building and openly sharing tools that predict which patients are most likely to have bacteremia and when a culture can be safely deferred. The simplest version works as a quick bedside score, no new software required.

From hand-hygiene audits to the SHEA Board of Trustees, the professional path of Alexander Sundermann, DrPH, CIC, FAPIC, AL-CIP, traces the arc of modern infection prevention. The former hospital IP—now a University of Pittsburgh assistant professor—pairs frontline experience with genomic epidemiology to turn sequencing into outbreak-stopping action.

Crowded waiting rooms can turn routine checkups into transmission hubs. Here’s how outpatient clinics can cut risk, starting at the front door, with smarter cleaning, hand hygiene, masks, and fewer extra visitors.

Hospital-wide sequencing of 8,567 Staphylococcus aureus isolates at NYU Langone revealed that many MRSA cases stem from tight community transmission networks—not in-hospital spread. Presented at IDWeek 2025, the work pinpoints distinct clusters (young MSM/substance-use networks, long-term care residents, and children) and urges IPC strategies that bridge hospital and community.

At IDWeek 2025, a Detroit consortium reported a familiar IPC paradox in skilled nursing facilities: Staff know the basics, but practice lags. Inconsistent rub times, dwell times, and respirator seal checks point to behavior-focused training—not more slides—as the next move.

A multifaceted infection-prevention push at a tertiary rehab ICU in the Upper Midwest reversed a rise in C difficile, lifting hand-hygiene adherence from 69% to 91% and cutting the C. diff standardized infection ratio from 1.6 to 0.4 over six months, researchers reported at IDWeek 2025 in Atlanta.

New IDWeek 2025 data show who C difficile kills most: White patients, women, and people in major metros—with most deaths tied to health care exposure—underscoring how basics and smarter antibiotics remain our best levers to cut mortality.

Candida auris is the pathogen that won’t take a hint—clinging to surfaces, nesting in biofilms, and outlasting rushed wipe-downs. Yet the chemistries potent enough to kill it can be punishing to people, devices, and environments. This piece tackles the tightrope: how to choose, use, and verify C auris effective disinfection without trading one risk for another.