Prevention
Latest News

Latest Videos

Shorts










More News


Antimicrobial resistance threatens all of modern medicine. Infectious disease expert Amesh Adalja, MD, FIDSA, senior scholar at the Johns Hopkins Center for Health Security, warns that health care workers face occupational exposure to drug-resistant bacteria. Judicious antibiotic use and policy reforms like the PASTEUR Act are critical solutions.

HSPA President Arlene Bush, CRCST, CER, CIS, CHL, SME, DSMD, CRMST, discusses certification advocacy, Capitol Hill efforts, workforce challenges, and why sterile processing is essential to patient safety, urging leaders to recognize and support the professionals behind every successful surgical outcome.

Health care–associated infections (HAIs) remain underestimated, driven by evolving pathogens, environmental reservoirs, and biofilm persistence. Experts argue outdated data and overreliance on hand hygiene obscure the true, growing burden of preventable infections.

Phase 3b ENCORE data show ARIKAYCE improves symptoms and culture conversion in newly diagnosed MAC lung disease, supporting earlier use. Findings suggest potential to shift treatment earlier and improve outcomes in this difficult-to-treat infection.


AI and agentic systems are transforming infection prevention by enabling real-time surveillance, predictive risk modeling, and earlier intervention, shifting health care from reactive response to proactive prevention and improving patient safety outcomes.

A former infection prevention professional shares his battle with MRSA and sepsis, revealing the lasting impact of health care–associated infections and why vigilance, accountability, and patient advocacy matter more than ever.

Marburg Virus Entry Mechanism Reveals New Targets for Antivirals and Infection Prevention Strategies
New research shows the Marburg virus enters human cells far more efficiently than Ebola, highlighting increased outbreak risk and underscoring the need for rapid detection, strict infection control, and novel antiviral development.

A national recruiter shares insights on infection prevention hiring trends, highlighting evolving background requirements, persistent RN bias, salary disparities, and the growing role of advocacy and data in shaping a more inclusive, competitive IPC workforce.

The global medical waste management market is rapidly growing, driven by healthcare expansion, regulations, and sustainability demands, transforming waste handling into a strategic priority for safer, more efficient, and environmentally responsible health care systems.

Tuberculosis affects 10.7 million annually. IPC professionals prevent health care-associated TB through respiratory isolation, staff screening, and contact investigation. World TB Day 2026 affirms TB elimination is achievable through dedicated infection prevention.

Sherrie Busby, steps out of dental IPC to highlight infection control risks in Alzheimers care, including UTIs, C difficile, and hygiene practices. Practical tips on handwashing, PPE, and environmental cleaning emphasize protecting vulnerable patients while supporting caregivers’ health and resilience in home settings and safety outcomes.

Peptilogics' PLG0206 represents a breakthrough innovation in infectious disease. First drug designed specifically to penetrate and kill biofilm-protected bacteria. RETAIN Phase 2/3 trial now enrolling patients with prosthetic joint infection. The previous phase showed 93% infection-free rate. It could revolutionize the treatment of medical device-related infections.

Ill-fitting PPE exposes women health care workers to infection risks, regulatory liability, and reduced performance. Wyatt Bradbury, MEng, CSP, CHST, CIT, TSSP, urges infection prevention leaders to assess fit, engage staff, and improve procurement practices to ensure safety, compliance, and equitable protection across clinical environments.

Federal court halts vaccine schedule changes, upholding evidence-based immunization practices. ICT reached out to key opinion leaders to find out their thoughts

Stethoscopes remain an overlooked vector for health care–associated infections. Infection prevention experts say inconsistent cleaning, workflow pressures, and cultural gaps contribute to contamination risks, especially for vulnerable patients such as those in oncology and emergency settings.

How IPC programs are shifting away from punitive audits toward human-centered coaching models. Include peer-to-peer observation, quiet feedback moments, and psychological safety as drivers of long-term adherence.

The Bug of the Month helps educate readers about existing and emerging pathogens that are clinically important in today's health care facilities.

AI is transforming hand hygiene monitoring by replacing limited manual observation with continuous, data-driven surveillance. New tools use computer vision and machine learning to detect sanitizer use and identify gaps in adherence.

Animal bites send millions to U.S. emergency departments each year, with risk rising during holidays and periods of increased household activity. This article examines bite-related infection risks, rabies exposure, and what infection preventionists can learn from seasonal trends to better protect patients and communities.

Improper linen handling in long-term care facilities can increase cross-contamination risk. Experts say laundry workflows, directional processing, and consistent wash parameters play a critical role in infection prevention by limiting microbial spread during the collection, sorting, laundering, and storage of contaminated textiles.

The COVID-19 pandemic has accelerated a shift away from droplet-based precautions toward a “through the air” framework that recognizes aerosol transmission across a continuum of particle sizes. As measles, SARS-CoV-2, and influenza circulate simultaneously, this article explains why ventilation, respirators, and higher air change rates must become core infection prevention strategies in health care facilities.
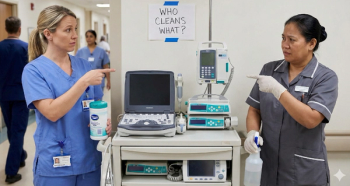
Shared medical equipment, such as IV pumps, workstations on wheels, and wheelchairs, often lacks clear cleaning ownership in hospitals. Experts say that defining responsibility, setting cleaning frequencies, and implementing verification processes can reduce the risk of cross-contamination and strengthen infection prevention programs without adding staff.

Congress Presses HHS to Release CDC Study on Reusable Health Care Textiles
Lawmakers are pressing HHS to release a CDC study on reusable health care textiles and PPE. Industry leaders say reusable gowns and linens could strengthen supply chains, reduce waste, and protect health care workers during emergencies, but the report remains unpublished.